





|

|
|
|

|
Search
12/11/2013
RESPONSES/COMMENTS (CLINICAL) - PART 1A
RE: Painful Foot Lumps
From: Bryan C Markinson, DPM. Robert P. Thiele, DPM
These are consistent with panniculitis of which erythema nodosum is one type. Do a 3 mm punch biopsy to the level of the fat. The specimen must include the fat. The TB status of the patient should also be checked. These lesions also may represent an atypical mycobacterial infection. Biopsy is best for definitive treatment.
Consider myxedema related to the thyroid disease. You can biopsy the skin of the mass and send it to a lab. E-mail a digital picture of the foot/leg mass to your lab along with a biopsy specimen and the medical history. I had a few similar cases. If you feel that the lesions are not that superficial, then perform incisional biopsy as you see fit. Let us know the results.
Robert P. Thiele, DPM, Hillsborough, NJ, drthiele@comcast.net
Other messages in this thread:
04/24/2025
RESPONSES/COMMENTS (CLINICAL) - PART 1A
From: Ron Werter, DPM
My suggestion is to take a course and get certified. Don’t screw around with it. The least you can do is be ineffectual, the worst is to cause damage.
A close friend of mine is an MD whose practice is exclusively prolotherapy. After 20 years doing this, he is still taking additional courses. I asked him about my doing this in my practice for heel pain. "Sure," he said, "but take the course. It’s not as simple as you think."
Ron Werter, DPM, NY, NY
03/03/2025
RESPONSES/COMMENTS (CLINICAL) - PART 1A
From: PM News Subscriber, David P. Luongo, DPM
This is a picture of my patient with T-cell lymphoma. A biopsy of your patient may be a good idea.
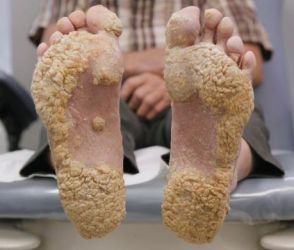 |
Plaque-Like Calluses on Weight-Bearing Surfaces |
PM News Subscriber
I've seen this before. For my patient, it was the onset of menopause where there was a sudden change in hormones. Have that checked out.
David P. Luongo, DPM, Paramus, NJ
08/09/2024
RESPONSES/COMMENTS (CLINICAL) - PART 1A
From: Jeffrey Kass, DPM
I’d like to thank Dr. Pressman for the free pearl. I sincerely appreciated the pearl and was ecstatic for the first time someone was not trying to extract money from me. I have also come across patients with palpable pulses who have had stenosis or occlusions and the pearl he has shared is of utmost value.
Jeffrey Kass, DPM, Forest Hills, NY
05/01/2024
RESPONSES/COMMENTS (CLINICAL) - PART 1A
RE: Functional Hallux Limitis
From: Jeffrey Trantalis, DPM
Howard Bonenberger, DPM hinted about a very important and prevalent condition that is seen in many, if not all, podiatry offices. This is hallux limitus. In the early 1980s, I had a professional NFL receiver come to me with hallux limitus. It was obvious that conservative treatment was the only option. At that time, orthotics with a hallux extension was the recommended treatment. So I tried this very treatment, knowing it would probably fail. Well it did fail.
At that time, I dispensed an orthotic where I increased the ability to plantarflex the first metatarsal by supporting the 1st metatarsal-cuneiform joint. This allowed for a more normal function of the first MPJ. This was very successful treatment that allowed the receiver to make his route maneuvers.
Jeffrey Trantalis, DPM, Delray Beach, FL
06/22/2023
RESPONSES/COMMENTS (CLINICAL) - PART 1A
From: Robert Kornfeld, DPM
Dr. Ribotsky implores me to "publish my outcomes". But not having lived in my shoes, he does not understand. I will explain. There are 2 parts to the story. 1) I adopted a more holistic paradigm in 1987 after a chronic illness (which could not be helped by any conventional doctors for a few years) was healed and resolved within 3 months of seeing a holistic internist. I experienced the power of natural healing firsthand. I dove into learning everything I could and began experiencing its power on my patients.
I wanted to share this with the profession so I spent a number of years lecturing about the things I do to assist my patients to heal. Although I was invited to speak a number of times at large podiatric conventions, my efforts were not being well received by the podiatric community. So I started trying...
Editor's note: Dr. Kornfeld's extended-length letter can be read here.
05/24/2023
RESPONSES/COMMENTS (CLINICAL) - PART 1A
From: Steven Finer, DPM, Walter Perez, DPM
Try increasing the Ativan to 2.5mg. or consider 10mg. of Valium which has a longer life. Watch out for interactions with other drugs. Also, patients sometimes complain of headache after Valium. It also has mild muscle relaxant properties.
Steven Finer, DPM, Philadelphia, PA
I have not prescribed anti-anxiety medication for a long time for any type of surgery, including bone surgery, but if I have a very anxious patient, I prescribe Valium 5mg, two tablets, and ask the patient to take one tablet with a sip of water 2 hours before the surgery and if still anxious the second tablet 1 hour prior to the surgery. But what I really believe helps the patient's anxiety is to prepare them for surgery thoroughly, explain to them what to expect at the surgical center or hospital, step by step, and address their questions and concerns. That will help patients stay more relaxed and comfortable. My advice is to spend time with the patient going through the surgery and the process, and you may not need anxiolytics. I try to avoid them and I usually let the anesthesiologist handle anxiety issues.
Walter Perez, DPM, Brooklyn, NY
05/04/2023
RESPONSES/COMMENTS (CLINICAL) - PART 1A
From: Thomas A. Graziano, DPM, MD, Alec Hochstein, DPM
There is not much history provided in the post regarding this "lesion" or even its duration. But in response to the poster question "any idea of what this might be?" I suggest a prudent approach would be first taking a biopsy of the lesion.
Thomas A. Graziano, DPM, MD, Clifton, NJ
In any seemingly healthy patient with a non-healing wound without specific etiology to point to for non-healing, a diagnosis of pyoderma gangrenous must be considered. Please keep us posted.
Alec Hochstein, DPM, Great Neck, NY
04/14/2023
RESPONSES/COMMENTS (CLINICAL) - PART 1A
From: Michael Orosz, DPM
I’ve recently started using a product from PediFix called Visco-Gel Hammertoe Crutch. These are especially effective for those patients with long toes that plantarflex over a crest pad.
Michael Orosz, DPM, Cedar Rapids, IA
01/09/2023
RESPONSES/COMMENTS (CLINICAL) - PART 1A
From: Robert Scott Steinberg, DPM
I have made ski boot-specific orthotics and have been doing custom boot fitting for over 30 years. I am a certified member of the Professional Ski Instructors of America, Rocky Mountain division. I worked with the Vail Ski School to refine the technique of using ski boot orthotics not only for support but to improve knee position and tracking. Making a proper orthotic for a ski boot differs from one for gait. When I put my running orthotics into my ski boot, my center of knee mass is misaligned!
I perform a full biomechanical exam. It is important to find any forefoot varus or valgus. Forefoot posting is all important. It determines the direction of knee travel, and it directly affects the alignment of the...
Editor's note: Dr. Steinberg's extended-length can be read here.
01/06/2023
RESPONSES/COMMENTS (CLINICAL) - PART 1A
From: Connie Lee Bills, DPM, John Rosselli CPed and Robert S. Schwartz CPed
I have adjusted orthotics for ski boots several times. It’s a much narrower shank and you have to grind the shell quite narrow. I use a functional sports-type orthotic with rearfoot intrinsic post to minimize bulk... 2 mm thickness forefoot extension.
Connie Lee Bills, DPM, Mount Pleasant, MI
Orthotics are essential! Shell selection is essential. Liners are less so, but our Surefoot custom liners are now so good, they double the life of a boot, and perform better (we use a patented memory foam that grips as tightly as the older foams, but have an elasticity that allows superior biomechanics). They are wired for heat, and pair with your phone. An orthotic that doesn’t fit in the footwear of its intended use will always be problematic, even if it’s otherwise perfectly designed.
John Rosselli CPed, Surefoot NYC, Robert S. Schwartz CPed, Eneslow
01/05/2023
RESPONSES/COMMENTS (CLINICAL) - PART 1A
From: Kevin B. Rosenbloom, C.Ped
Regardless of the type of skier, of type of skiing, a custom orthotic or insole that fits the shape of the plantar aspect of the foot in a neutral position will improve the comfort and performance. From your orthotic lab, you will need to request a narrow or ski-specific orthotic to fit into ski boots, a heel cup that is approximately 10mm (12mm for mens boot size 11 or larger) and a top cover that allows the foot to slide in and out easily for recreational skiers, i.e. vinyl or Protex. For advanced skiers, an EVA or Prolite top cover is recommended for better connection and less slipping within the boot.
Similar modifications can be made in the rearfoot, such as skives or rearfoot posts to help maintain the subtalar joint near neutral. The midfoot or arch of the orthotic should be full contact with the midtarsal joint in neutral. The forefoot of the orthotic generally does not require such things as met pads or off-loading pads because there are no propulsive or dorsiflexion moments loaded on the forefoot tissues. If a patient has forefoot modifications, I recommend foregoing them in a ski boot unless chronic pathology is present.
The modification pads often take up needed room within the toebox. Consider the boot shop that sold the patient the boots. If it has a reputable boot fitter, the patient will have had some custom insoles or OTS insoles provided by the boot fitter. Some are good and some less effective than a neutral impression that can be taken in your office and fabricated by your lab. If you can, send the boot liners or boots to your orthotic laboratory so the lab can fit the orthotic to the boot to make your life easier dispensing to your patient.
Kevin B. Rosenbloom, C.Ped, CEO, KevinRoot Medical
11/18/2022
RESPONSES/COMMENTS (CLINICAL) - PART 1A
From: Elliot Udell, DPM
When I first attended podiatry school, back in the '70s, the main treatment for verrucae, including mosaic verrucae, was topical Sal acid and weekly debridement. Dermatologists and some podiatrists added on liquid nitrogen therapy. Over the years, there have been credible studies showing that Sal acid treatment is 70% effective. Our problem is how to handle the 30% of the patients who are not responsive and are likely to travel to multiple podiatrists seeking a cure.
Unless you want to believe the vendors promoting drugs and surgical therapies, who will tout their products as being cure-alls for warts, we have to face the reality that when it comes to warts, we are still playing with the same deck of cards in 2022 as we were in 1978. Some new and old treatments work for some patients and not for others. In our office, when one treatment fails, we try another. We will either succeed or the patient will move on to another doctor. As Dr. Sullivan writes, there isn't a wealth of literature proving that any one treatment is the be-all and end-all for treating all verrucae.
Elliot Udell, DPM, Hicksville, NY
10/27/2022
RESPONSES/COMMENTS (CLINICAL) - PART 1A
From: Russell G. Volpe, DPM
I suggest that this 3-year-old with a "painful port-wine stain" might have pain for some other reason in the foot unrelated to the port-wine stain. Take a look at foot mechanics, superstructural alignment and potential compensation as possible sources of discomfort or pain in the area. The location of the symptoms in the "proximal arch" makes me suspicious that biomechanics may be at issue here, and the coincident location of the port-wine stain may be a distraction.
As a podopediatrician, I see many children with unusual and highly variable presentations of pain, discomfort, and activity alterations that are a result of faulty lower extremity mechanics. In younger children, these can be particularly challenging to work up as information about the complaint from the child is often vague and inconsistent.
Russell G. Volpe, DPM, NY, NY
10/06/2022
RESPONSES/COMMENTS (CLINICAL) - PART 1A
From: Brian Lee, DPM, Lance Malusky, DPM
I had a very similar situation many years ago. Don't bother trying to numb the toes. If you're good and efficient, you can do a partial avulsion in literally 5 seconds. I did that and the ingrowns resolved quickly. I saw her again as a late teenager for something else but her toenails were never a problem again. Problem solved.
Brian Lee, DPM, Mt. Vernon, IL
I have treated a few patients this young over the years. The bigger problem is the over-protective parent. The question of hospital management is expense, and many anesthetists may not have the patience to be kind. My office technique involves managing the parents' expectations of painless surgery. To numb the toe, a calm parent, and a less distraught friend is utilized. One person holds the ankle while the other reassures the child that all is well. The physician then uses ethyl chloride spray and a hallux V-block. After a few moments, the ankle holder is shown that the toe is numb by poking the toe with a semi sharp instrument with no response from the child. A slant back may be considered, but recurrence is at risk, considering that this clinical picture suggests a permanent anatomical medial border curvature. Only if both borders show that, would the lateral borders be corrected; if lateral paronychia without curvature is seen, a minor slant back only, with curettage of granulomatous tissue is considered.
The usual surgical approach is with an English anvil nail nipper, and then a #61 mini Beaver Blade, which splits the nail plate to the matrix zone. Remove the offending nail with a small straight hemostat. A culture and sensitivity can be considered. Inspect under the posterior nail groove for any cutaneous debris that might cause a later foreign debris reaction. Standard phenol Q-tips are useless. Instead, a flat toothpick with a wisp of cotton is spin-loaded. 2 X 20 seconds phenol is utilized, rolling the same direction that the cotton was loaded. Dab away any excess phenol before lavage. Dress as usual.
Lance Malusky, DPM, Dayton, OH
08/18/2022
RESPONSES/COMMENTS (CLINICAL) - PART 1A
From: James C. Ricketti, DPM, Lance Malusky, DPM
The original studies performed at Lehigh University by Dr. Nabolah showed that only one application of the Phenol EZ Swab was needed to destroy the matrix. We have marketed that fact for over 31 years.
Disclosure: I am the original inventor of the Phenol EZ Swabs
James C. Ricketti, DPM, Hamilton Square NJ
For chemical matrixectomies, I was taught by my program manager, and used, 3 x 30 seconds phenol (88%) applied with a debulked Q-tip. We also "neutralized" it with saline. I would consider a 2 x application, but sometimes the first application would reveal blood on the Q-tip, suggesting that the initial application was effectively diluted.
Also note that Phenol-EZ Swabs, while an acceptable quality product, was too generous and could cause spill-over chemical burns. We ordered phenol in bulk from a medical distributor, with the usual shipping hazard fee, and poured it into a 1 oz. brown drug jar. Gloves and a running sink were on the standby for safety.
Lance Malusky, DPM, Dayton, OH
04/21/2022
RESPONSES/COMMENTS (CLINICAL) - PART 1A
From: Michael M. Rosenblatt, DPM
The so-called "Covid Wound", a rather horrifying slough of tissue on the dorsum of the foot that exposed the extensor tendons, allegedly is the result of a "mixed 4% absolute alcohol and steroid in the same syringe." This is highly unlikely. The most logical explanation is that the dilution was incorrect and undiluted absolute alcohol was administered. This combined in a patient with very poor circulation in the foot might be the reason for that dreadful result.
It is even possible that the solution injected was not actually alcohol but undiluted phenol or an unidentified full-strength toxic anhydrous solution. When an unexpected result occurs, the first place you look for is operator error. Nowhere is it more evident than in this case.
Michael M. Rosenblatt, DPM (Retired), Henderson, NV
04/19/2022
RESPONSES/COMMENTS (CLINICAL) - PART 1A
From: Robert Scott Steinberg, DPM
I am disappointed by Dr. Cassidy's post. He put medical care aside and pushed what seemed to be his anti-vaccine and political agendas.
I had my second booster three weeks ago, and the sun came out today post-vaccination. Oy!
Robert Scott Steinberg, DPM, Schaumburg, IL
04/15/2022
RESPONSES/COMMENTS (CLINICAL) - PART 1A
From: Bryan C. Markinson, DPM, Richard Rettig, DPM
This patient needs a vasculitis/collagen vascular work-up immediately by a rheumatologist. Even though pulses are palpable, a vascular evaluation is also indicated. Also consider colonoscopy for inflammatory bowel disease and a hematology consult as well. Until all that is done, I would keep COVID-19 at the bottom of the list. A wound biopsy may be helpful.
Bryan C. Markinson, DPM, NY, NY
The wound looks quite familiar to me. It looks like a bad "miss" from a heroin injection. There is lots of tissue destruction, poor healing, but no actual infection. You describe scabs up and down the legs...those are from 'better' injections. You describe her stench of smoke despite admitting to 5 cigarettes a day - so you suspect she is lying about her social history. The edema in the other leg is from the newer injections. "COVID-19 wound" should be low on your differential.
Richard Rettig, DPM, Philadelphia, PA
07/14/2021
RESPONSES/COMMENTS (CLINICAL) - PART 1A
From: Stephen Kominsky, DPM
This is the time where I am forced again to climb down from my dinosaur and onto my soapbox; Dr. Samuel was eloquent and complete (and correct) with his recommendations on how to address this patient surgically EXCEPT for one thing. He referred to the Lapidus procedure as a Lapiplasty as if that is the actual procedure, when in fact, the Lapiplasty is a “brilliant” marketing campaign which requires the surgeon to use a series of instruments to achieve a predictable outcome. An analogy would be appendix surgery. The technique is an appendectomy, whether it is done laparoscopically or as an open procedure.
There is absolutely nothing wrong with this system; in fact, I love it, but “the Lapiplasty" is not a procedure. It is a technique for doing a Lapidus procedure. Semantics, maybe. Call me old.
Stephen Kominsky, DPM, Washington, DC
07/13/2021
RESPONSES/COMMENTS (CLINICAL) - PART 1A
From: Chris Seuferling, DPM
As always, treat symptoms not x-rays. It wasn’t clear if the bunion itself is painful or not? In lieu of this information and other pertinent clinical information, I would recommend 1st MPJ arthrodesis and 2nd metatarsal Weil osteotomy (with lateral translation of methead). I believe traditional bunion procedures would be difficult with this patient’s met adductus. Also, 1st MPJ fusion would give her solid 1st ray to prevent lateral transfer symptoms.
Chris Seuferling, DPM, Portland, OR
04/19/2021
RESPONSES/COMMENTS (CLINICAL) - PART 1A
From: Peter J. Bregman, DPM, Kenneth Meisler, DPM
It sounds like a duck (Morton’s neuroma) so likely it is. If steroid injections did not cure the “bursitis” then maybe it is not that. MRIs are great but not always right, especially with diagnosing MN. If this were my patient, I would say we are going to the OR for a decompression of the nerve and if I see a bursal sac in there, I will remove it. Unless the bursal sac is plantar to the deep transverse ligament, there should not be any walking on a pebble feeling. Maybe there could also be a plantarflexed metatarsal head there as well.
Peter J. Bregman, DPM, Las Vegas, NV
I would refer the patient to someone experienced in ultrasound-guided injections. Injecting directly into the bursa is usually successful.
Kenneth Meisler, DPM, NY, NY
04/06/2021
RESPONSES/COMMENTS (CLINICAL) - PART 1A
From: Burton J. Katzen, DPM
In response to Dr. Blanken's response concerning 3rd metatarsal osteotomies for 2nd innerspace neuroma, I suggest that prior to stating in a public forum that I possibly perform unnecessary surgery with possible severe iatrogenic complications, while also questioning my integrity, I suggest that, due to his obvious inexperience with the procedure, he do a little research.
I hope the these links: article 1, article 2 will help to educate him. The positive results have shown to be up to 93%, actually an improvement from the DTML or actual neuroma excision. Of course, performed using MIS techniques, the recovery period is less than described in the articles.
Burton J. Katzen, DPM, Temple Hills, MD
03/17/2021
RESPONSES/COMMENTS (CLINICAL) - PART 1A
From: Clifford Wolf, DPM,Chris Seuferling, DPM
Turf toe is an injury to the 1st MPJ. Its etiology is not neuro-mechanical. Are you referring to another condition called turf toe/hallux limitus?
Clifford Wolf, DPM, Oceanside, CA
I presume Dr. Dananberg's treatment recommendations are referring to "functional" hallux limitus and not for a 1st MPJ with moderate or advanced arthritic changes? In my experience, these latter patients are often in more pain with MOVEMENT and DO benefit from carbon fiber plates...and sometimes surgery is indicated.
I'm curious what Dr. Dananberg recommends treatment-wise in these arthritic cases?
Chris Seuferling, DPM, Portland, OR
03/09/2021
RESPONSES/COMMENTS (CLINICAL) - PART 1A
From: Ben Pearl, DPM
I do not advocate substituting diagnostic ultrasound for x-rays, but it does offer a more expeditious adjunct study for the astute practitioner who has ultrasound in their office. I have used it for identifying plantar plate tears, flexor tenosynovitis, and stress reactions of the sesamoids. In recent communications with John Cozarelli, DPM, he has suggested a histogram to assess degenerative changes in the tendon and capsule apparatus quantitatively. If your existing unit does not have the software capabilities to assess and measure the degree of heterogeneity within these structures there are overlay programs that exist to measure changes in serial ultrasound images.
Ben Pearl, DPM, Arlington, VA
02/22/2021
RESPONSES/COMMENTS (CLINICAL) - PART 1A
From: Charles Morelli, DPM, Ben Pearl, DPM
Thank you Dr. Ross for mentioning Viagra as something to be concerned with regarding a patient's blood pressure as it is a vasodilator and pressure can be affected, as it had slipped my mind. He reminded me that I also have suggested both Viagra and Cialis to both male and female patients as a potential first-line defense against symptoms associated with Raynaud’s due to the very fact that they are vasodilators. You will get some raised eyebrows, but once you explain its mechanism of action, it is taken seriously and these patients will do almost anything to address their pain and reduce their chances of potential serious complications.
Charles Morelli, DPM, Mamaroneck, NY
I would add the use of a high-quality thin wool sock. A vascular interventionalist I know uses Viagra in very low doses, but I have not tried this for patients yet and agree with a cautionary advice about using dual treatments that can cause hypotension.
Ben Pearl, DPM, Arlington, VA
|
| |

|
|
|







