04/24/2026
QUERIES (CLINICAL)
Query: Source for Hyfrecator for Partial Nail Matricectomies
I appreciate the feedback from everyone. For those who have had success with radiofrequency, would you be able to share the specific brand unit you have used? The only one I have come across in my research that was geared towards podiatry was from Ellman, which has been discontinued as of 2024.
Anas Khoury, DPM, Passaic, NJ
04/20/2026
QUERIES (CLINICAL)
Query: Hyfrecator for Partial Nail Matrixectomies
I’m looking for advice/feedback regarding using a hyfrecator for partial nail matrixectomies versus phenol/alcohol. I would appreciate procedure protocols, outcomes, and pros/cons.
Anas Khoury, DPM Passaic, NJ
04/01/2026
QUERIES (CLINICAL)
Query: Source for Monochloroacetic acid 80%
I am writing to inquire if any subscribers or advertisers can recommend suppliers for Monochloroacetic acid 80% used in wart treatment. I am currently looking for companies that carry this specific concentration.
David Chung, DPM, Aloha, OR
03/13/2026
QUERIES (CLINICAL)
Query: Bleomycin Injections for Verrucae
Is anyone using bleomycin injections for verrucae? What is your protocol and success rate?
Brian Kiel, DPM, Memphis, TN
08/26/2025
QUERIES (CLINICAL)
Query: Recommended Time Period Between Neuroma Injections
What is the recommended time period between multiple (3) injections for treating neuromas? Each injection is 3cc containing equal parts of: 1% Xylocaine, Kenalog, and Vitamin B12. Orthotics, with the appropriate placed neuroma pads, are also dispensed.
Kel Sherkin, DPM, Toronto, Canada
08/16/2025
QUERIES (CLINICAL)
Query: Infection Post-Repair of Ruptured Achilles Tendon
A 69 year old female with a PMH of RA ruptured her tibialis anterior tendon at the insertion. She takes methotrexate, plaquenil, and sulfasalazine, along with monthly Orencia infusions, but has held off on the infusions since her surgery 4 months ago. Repair was performed with Arthrex suture tape, anchoring it with a bioabsorbable Swivelock anchor. This was reinforced with a Wright GraftJacket wrap since the tendon was quite damaged. Unfortunately, she has developed a draining 2mm sinus tract at the incision and presumably has infection within either the graft, the suture, or both.
X-rays do not show any concern for bone erosion. Cultures have grown staph hominis and she has been on appropriate IV antibiotics directed by ID for 6 weeks with no resolution. I was contemplating doing a limited debridement of the sinus tract and an adjacent graft or visible suture fibers, possibly dropping some Vanco powder there in an attempt to eradicate this infection. I know there is no way to remove the entire graft and suture without compromising the tendon and giving her drop foot. I did a long Krackow suture to secure it, which is deeply buried within the tendon and bone anchor. She has minimal pain, is active, and is walking about 7 miles/day for exercise. I am just trying to do anything to avoid sacrificing the tendon and would appreciate any advice.
08/05/2025
QUERIES (CLINICAL)
Query: The Use of Injectable Hyluronidase Gel for Arthritis of the Feet
For decades, orthopedists and other medical specialists have been injecting hyluronidase gel into knees. There have been a few papers published suggesting that this can be helpful with arthritis of the foot and ankle. Question: How many of you have used this for foot and ankle arthritic conditions and does insurance cover it for foot and ankle osteoarthritic conditions?
Elliot Udell, DPM, Hicksville, NY
06/20/2025
QUERIES (CLINICAL)
Query: Management of Fryberg’s Infraction
My patient is a 13-year-old diabetic female who is a very active soccer player. She recently went through a nutritional issue as she was bulimic for about six months. This has been managed and she’s doing well. She showed up to my office with pain into the third and fourth metatarsal heads and we have an MRI that’s consistent with acute Fryberg’s infraction. I would be very interested to hear how people have managed this.
06/12/2025
QUERIES (CLINICAL)
Query: Hyluronidase for Scar Tissue
I have a patient who is suffering from chronic pain from what I think is scar tissue at the first branch of the lateral plantar nerve. It is affecting the quality of their life. They had surgery for removal of an accessory soleus that was causing pain but it left them with scar tissue causing nerve entanglement. This has been confirmed by post-operative MRI. Local blocks, multiple shots of cortisone, desiccated alcohol, and most recently D5W perineurial injections have all failed in fact some have exacerbated the problem.
She came to see me to discuss hyluronidase injections into the scar tissue to see if that would help. She is vehemently opposed to any other surgery which I don’t blame her. She is a good patient and has reasonable expectations. Does anyone have experience with the use of hyluronidase to reduce scar tissue and what protocols and dosages are being administered?
06/06/2025
QUERIES (CLINICAL)
Query: Taking Blood Pressure Prior to Minor Procedures
I’d like to ask a question about an incident that occurred the other day. I was excising a painful hyperkeratotic lesion from the 5th toe lateral proximal nail fold with lidocaine plain. During the excision of this 3 mm lesion, bleeding did not stop for more than 30 minutes. I decided to take her blood pressure which was 206/104. I assumed her BP was causing this bleeding issue since she was not on any anticoagulants, no hematologic pathologies as per her PCP.
I’d like to ask if we should take BPs on patients we are doing any procedure on as minor as this is. P.S. the bleeding finally stopped, but I did send her to the ED which confirmed hypertension as well. The lesion was sent for pathology.
Name Withheld
06/03/2025
QUERIES (CLINICAL)
Query: Short Proximal Phalanx
Over the 36 years of surgery, I have done many osteoclasis procedures on metatarsals—but never on a proximal phalanx alone. A gradual lengthening is preferred over a single stage lengthening due to vascular concerns.
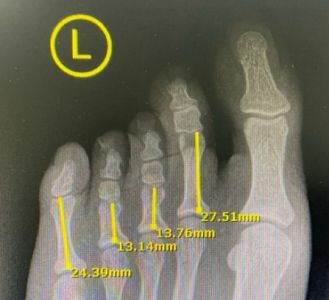 |
Short Proximal Phalanx |
I am planning to place the proximal pins in the metatarsal and the distal pins in the distal aspect of the proximal phalanx. I am open to comments and suggestions.
05/16/2025
QUERIES (CLINICAL)
RE: Unusual Surgical Suture
Gary Smith, DPM
I saw a patient this week who showed me their hernia repair incision 3 weeks post-op. The incision had been closed with 10 external horizontal mattress sutures with what appears to be 2-0 Vicryl. The incision seems fine but the patient is still having inflammation and drainage around the sutures in the knot areas above the incision. The patient has been getting it wet in the shower since Day 2 as allowed by their surgeon. I have never heard of absorbable sutures being used like this. It seems to me they are providing a portal for moisture and bacteria to enter the skin. The knots are yellow and look like bacteria farms. Is this something new? Has anybody ever heard of this?
Gary Smith, DPM, Bradford, PA
04/23/2025
QUERIES (CLINICAL)
Query: Concentration of Dextrose Solution for Prolotherapy?
Does anyone have any experience in prolotherapy for lower extremity conditions. What concentration of the dextrose solution do you find to be the most effective?
Brent Rubin, DPM, Lakewood Ranch, FL
04/07/2025
QUERIES (CLINICAL)
Query: Invisible Metallic Fragments (Morgellons Disease?)
A middle-aged female patient presented with a complaint of an embedded metallic shard in one of her feet after walking barefoot on a garage floor, even though she felt no puncture or injury at that time. She had attempted self removal of the foreign object with a scalpel several times prior to the initial visit. On exam, there was a single tiny 1 mm reddish macule. X-rays did not show any metal or other visible foreign body. She was convinced of its presence and stated the fragment must be too small to be seen on the x-rays.
I performed an exploratory I&D of the macule and nothing was found. She returned a month later stating that the problem was still there, causing pain; and now she had it in the other foot as well. She stated she had removed a couple of tiny black filaments herself and could not understand why I couldn't see them. An exam again showed a couple of tiny red macules. Less aggressive trimming/enucleation of the macules yielded nothing. I researched this and came across Morgellons disease, a psychiatric disorder, which seems to fit. Has anyone else encountered this? Any suggestions for treatment?
Name Withheld
02/28/2025
QUERIES (CLINICAL)
Query: Plaque-Like Calluses on Weight-Bearing Surfaces
A 19 year-old Hispanic female patient presented with plaque-like calluses on the weight-bearing surfaces (balls and heels) of BOTH feet which started a month after starting a new job at a memory care facility. Her new job consists of helping folks with bedtime routines, (wears/changes gloves routinely), and wiping/cleaning residents and repositioning them as needed. Shortly after the skin changes on her feet occurred, her fingernails started to become discolored, pitted, dystrophic and thickened with dark longitudinal streaking, starting with the right thumb nail. Her toenails look fairly normal with no obvious signs of fungal infection.
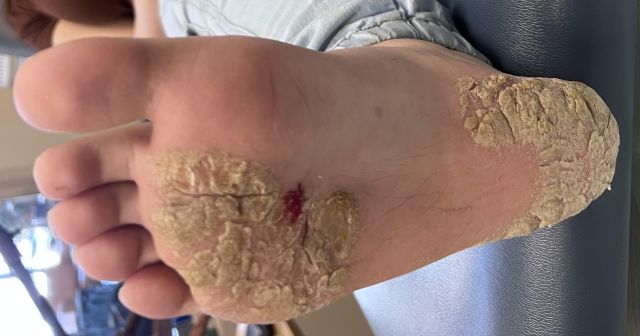 |
Plaque-Like Calluses on Weight-Bearing Surfaces |
This seems to be auto-immune driven, however, given the sudden onset with the new job and heavy use of gloves, I have some concern for infection, either fungal or bacterial. We have started her on antifungals to see if this helps. A dermatologist has suggested hereditary palmoplantar keratoderma, recommending symptomatic treatment with inserts and urea cream. A biopsy is being considered, but first utilizing supportive inserts to reduce stress/weight on the weight-bearing surfaces. Additionally, she will start applying urea cream to one foot, triamcinolone to the other, and see what results we get. Of interest, the patient also has a history of loop bowel in addition to scoliosis and eczema. No skin changes to the knees, back, neck, etc., although she has a very dry scaly scalp. Psoriasis is a consideration. Input and suggestions are appreciated.
01/27/2025
QUERIES (CLINICAL)
Query: AV Malformation
My granddaughter was diagnosed with an AV malformation in her foot, located around the plantar aspect, slightly distal to the calcaneal tuberosity. She is 11 years old and has been dealing with this for around two years. Because of the difficult location being against the nerve and artery, my daughter and son-law were advised to try sclerotherapy by an interventional radiologist. This was done twice at CHOPS in Philadelphia. Neither attempt gave relief to my granddaughter.
The latest MRI which was done this week showed the AVM was slightly more flattened than the last MRI and involved the flexor digitorum brevis and quadratus plantae muscles. Also noted was edema of the diaphysis of the 2nd metatarsal which has developed since the previous MRI. The marrow of the 2nd metatarsal is heterogeneous and may reflect an infarct or be indicative of stress. If anyone has dealt with this condition and can give some input or doctor recommendations, I would greatly appreciate it.
Name Withheld
12/09/2024
QUERIES (CLINICAL)
Query: Can a Nail Like This Ever Regrow Normally?
Below is a photo of a thick abnormal toenail that all of us have come across in practice. The nail oftentimes stops growing distally as it comes to a dead end of hitting skin that is raised above the level of the toenail.
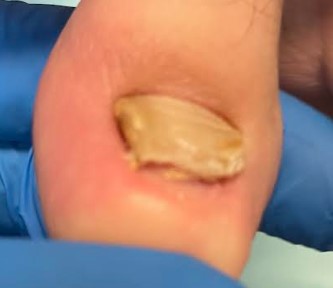 |
Can a Nail Like This Regrow Normally? |
Is there any way to make this mail grow normally again?
12/05/2024
QUERIES (CLINICAL)
Query: Treatment of Onychomycotic Onycholysis
Below is a photo of a toenail which is no longer centrally attached to the nail bed. The nail is arched away from the nail bed. Under the arch there is nail fungus growing on the nail bed. I was wondering if any colleagues have any “pearls” in successfully treating this condition in order to bring back a normal toenail.
 |
Onychomycotic Onycholysis |
I realize removal of the toenail and allowing it to regrow may be an option. My concern there is causing a case of “disappearing toenail syndrome” which some may find more unsightly than the current state this toenail is in.
10/10/2024
QUERIES (CLINICAL)
Query: Jublia Reaction
A patient was prescribed Jublia by his PCP. A few weeks later, he presented at his PCP with this reaction due to the daily application of Jublia as directed.
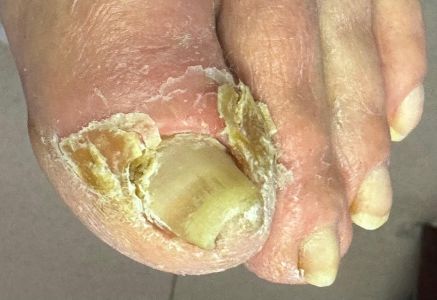 |
Jublia Reaction |
The PCP said, "see your podiatrist for an opinion." Has anyone seen this reaction to Jublia?
08/08/2024
QUERIES (CLINICAL)
Query: Lichen Planus
A patient presented with a dermatological disorder affecting multiple areas of his body including his face. His dermatologist did a biopsy and diagnosed it as lichen planus. Below is a photo of it.
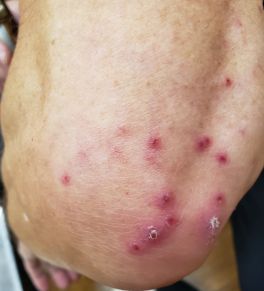 |
Lichen planus |
He said that he absolutely has no pruritis. The cases I have seen throughout my career always presented with severe itching and that is what brought the patient into my office. Could the dermatologists be missing something?
07/29/2024
QUERIES (CLINICAL)
Query: Transient Discoloration of Fingernails
A 46-year-old type two diabetic, BMI of 31, has been on testosterone therapy for a few years and has recently been taken off therapy. He has been having some generalized neuropathy complaints in his legs, however he has discoloration on the sides of his fingernails but nothing on his toes.
 |
Transient Discoloration of Fingernails |
He states that this will appear for a few months and then go away and come back. It is not painful. He has tested positive for ANA with a pattern consistent with lupus a few times. His rheumatologist did not think it was worth treating. Any input or thoughts if you recognize what’s going on in his fingers that might be contributing?
07/26/2024
QUERIES (CLINICAL)
Query: Balance Braces
Almost every DME company has their own version of a "balance brace". I was wondering if anyone can answer a few questions for me. The brace is often touted at seminars as part of a fall prevention protocol. Question 1) Is there any proof at all in the medical literature that wearing of this brace prevents falls? (I am not asking if it decreases postural sway).
My second question is from a biomechanical standpoint, the brace cuts down on sagittal plane motion of the ankle as there is a stationary plate under the device - is this truly beneficial over allowing sagittal plane motion? In other words, is there any proof that this configuration of the brace is more beneficial for fall prevention than a typical split upright AFO?
Jeffrey Kass, DPM, Forest Hills, NY
07/15/2024
QUERIES (CLINICAL)
Query: Acute Peroneal Longus Tear/Surgical Case
A 63 year old well-controlled DM type 2 active male was playing golf and felt a "pop" in his lateral right ankle after finishing his swing. There was no inversion sprain and the patient did not fall before or after the injury. The pain was initially +8/10. He was unable to bear weight. He went to an ED. X-rays were negative. A modified Jones dressing was applied; crutches rest, elevation, and ice relieved symptoms to a 90% improvement. An MRI was ordered by the ED that was done 5 days after the injury revealed a completely torn peroneal longus tendon retracted to the lateral calcaneus. Old AFTL and CFL tears were noted as well. The brevis was normal.
Physical exam revealed intact sensation and palpable pedal pulses. There was edema laterally with minimal to no ecchymosis, +4/5 eversion without pain. The patient states tha he has almost no pain and no trouble walking with normal ADLs. He wants to know if the operative repair can be delayed until the fall. I discussed muscle atrophy of the PL with delaying operative repair. I'd like to know the opinion of my colleagues. I'd appreciate any input.
05/20/2024
QUERIES (CLINICAL)
Query: Men’s Shoe Recommendations Post-Achilles Tendon Rupture
What are the best men’s shoe recommendations post-Achilles tendon rupture and repair?
David Cohen, DPM, Pikesville, MD
03/21/2024
QUERIES (CLINICAL)
Query: Podiatrist with Carpal Tunnel Syndrome
I have recently been diagnosed with carpal tunnel syndrome. A recent post mentioned that radial pulse therapy has been used to successfully treat trigger finger. Has anyone had experience in using this for treatment of carpal tunnel syndrome?
Name Withheld







