





|

|
|
|

|
Search
12/19/2016
RESPONSES/COMMENTS (PM ARTICLES)
From: Don Peacock, DPM
I've had the opportunity to perform the Katzen modified version of the MIS Wilson osteotomy. The procedure is very effective in some patients. I use the procedure in mild to moderate bunion deformities with mild PASA and a relatively small bunion/ "bump". I do agree with Dr. Greenberg and Kass with respect to head-to-head x-ray evaluations. The excellent surgical result from Dr. Cohen is in the early post-op stages and it is obvious that the patient is guarding in the post-op. Here is a patient whom I performed the procedure on, including a weight-bearing pre-op AP view along with a six week post-op view.
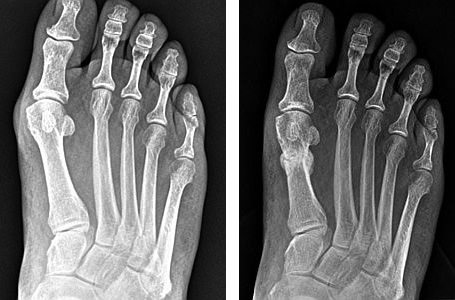 |
Pre- and post-op weight-bearing AP views |
In these views, we're seeing the deformity correction further out and the patient is not guarding as much in the post-operative views. Secondary bone healing is seen at this stage and good anatomical, clinical, and subjective results were achieved. The pre-op IM angle is 13 and the HA angle is 22. The post-op IM angle is 8 and the HA angle is 11.
Don Peacock, DPM, Whitesville, NC
Other messages in this thread:
02/04/2026
RESPONSES/COMMENTS (PM ARTICLES)
From: Allen M. Jacobs, DPM
Dr. Orosz is correct; lipedema is yet another potential cause of lower extremity edema. Lipedema is “classically” non-pitting and, therefore in theory, likely less responsive to compression therapy. However, lipolymphedema, like phlebolymphedema, is now a recognized clinical entity. As such, a secondary diagnosis of lymphedema concurrent to that of lipedema may be appropriate, thus qualifying the patient for benefits of the Lymphedema Act and thus helpful to the patient from a psycho-social and physiologic aspect.
Allen Jacobs, DPM, St. Louis, MO
02/03/2026
RESPONSES/COMMENTS (PM ARTICLES)
From: Michael Orosz, DPM
I would like to thank Dr. Jacobs for his thorough review of the complexity of evaluation and treatment of lower extremity lymphedema and PVD/PAD. To make things more complicated, podiatrists should also be aware of lipedema as a cause of swelling and enlarged tissue in the legs, thighs, and even the upper extremities. I suggest visiting the Lipedema Foundation website at lipedema.org to learn more.
Michael Orosz, DPM, Cedar Rapids, IA
01/31/2026
RESPONSES/COMMENTS (PM ARTICLES)
From: Allen M. Jacobs, DPM
The recent discussion of the Lymphedema Act and the ability of the podiatric physician to be reimbursed for the dispensing of certain products such as compression garments as an aid for the management of lymphedema is helpful for understanding the economic and coding aspects of lymphedema. However, I believe the clinical issues discussed in this article require a more detailed and accurate discussion.
Editor's note: Unfortunately, this extended-length letter which appeared in the 1/29/26 issue of PM News included only the first part of Dr. Jacob's response. To read the entire letter, click here.
12/08/2025
RESPONSES/COMMENTS (PM ARTICLES)
From: David Secord, DPM
I thought that I’d offer a correction in the published “Implications of Cannabis Use on Diabetes and Diabetic Ulcers It’s important to understand its use in wound healing,” by Zanib Cheena, DPM, MS and Stephanie Wu, DPM, MSC.
In that article, they state that “According to the Center for Disease Control (CDC), cannabis is the most commonly used federally illegal drug in the United States as it is currently legal in 24 states for recreational use and in 40 states for medical use.” Marijuana is still a Schedule I narcotic and is not legal in any State of the Union. It has been decriminalized in these states, but it is still a felony to grow, process, sell, and distribute or possess this...
Editor's note: Dr. Secord's extended-length letter can be read here.
08/25/2025
RESPONSES/COMMENTS (PM ARTICLES)
From: Rod Tomczak, DPM, MD, EdD
I have two daughters who are physician extenders, but I can’t simply define what a physician extender really is. Ludwig Wittgenstein, an analytical philosopher, said in 1953, “The meaning of a word is its use in the language.” That certainly clears it up.
It seems an extender is now able to perform a task or interpret some evidence and act on it in a realm that previously was limited to a physician. A CRNA provides anesthesia for our patients. They act independently except during induction and emergence when the anesthesiologist is required to be present in the operating room according to most state laws. You and I know that is not always the case. State laws limit the number of ...
Editor's note: Dr. Tomczak's extended-length letter can be read here.
08/22/2025
RESPONSES/COMMENTS (PM ARTICLES)
From: James Hatfield, DPM
I enjoyed reading Dr. Jon Hultman’s article in the August 2025 Podiatry Management. I couldn’t agree with him more. Podiatry has missed the boat or has been late for the boat historically. Let’s talk about radiology. No podiatrist would think of practicing without x-ray facilities in their office now – but it wasn’t always the case. We’re all familiar with Dale Austin via his bunionectomy (technically the Austin-Leviton bunionectomy - or Chevron, if you’re an orthopedist). Dale Austin was a podiatrist in the Los Angeles area in the 1950s and decided to do something really radical. He was the first podiatrist in the state to have an x-ray machine.
You’d think the other podiatrists (then chiropodists) in the area would applaud him – but just the opposite. They were appalled and angry. They were afraid that the orthopedists who sent palliative care to them would stop referring. Dale Austin became frustrated by this response and decided to go back and become a DO. Then, in 1961, via legislation, the DOs agreed to merge with the MDs in California, so he became an MD, though he still practiced primarily foot care. Too bad for podiatry.
Dr. Hultman is right about having a form of certified podiatric hygienist in the office. There’s a huge number of palliative patients who will need surgical services at some point and it would obviously be optimal if these patients could be cared for in a podiatry practice rather than somewhere else. And, as Dr. Hultman pointed out, it pays. Let's not miss the boat again.
James Hatfield, DPM, Encinitas, CA
08/16/2025
RESPONSES/COMMENTS (PM ARTICLES)
From: Elliot Udell, DPM
Dr. Kaufman asks a pertinent question. If podiatry schools are not filling their classes, why are new schools opening? Why are they staying open?
Podiatry colleges are independent entities. Some are private and others are part of large universities. No one can wave a wand and decide to close any of these schools. If a class is not filled but the university or college is making out well financially with tuition and donations, there is no incentive for them to close, even if they only have "five students." On the other hand, if the finances of these institutions "go South," they may be forced to close, and here again, no one in our profession will have any say over that decision.
Elliot Udell, DPM, Hicksville, NY
08/15/2025
RESPONSES/COMMENTS (PM ARTICLES)
From: Heather Kaufman, DPM
I read "Our House is On Fire!" (June/July 2025). I am wondering if anyone has addressed the elephant in the room which is that if the numbers are going down, then why in the past five years have new podiatry schools opened? LECOM opened their podiatry school in 2022 and UTRGV opened theirs in 2022 as well. If the numbers were low to begin with, why dilute the dwindling applicant pool further by adding more seats to fill? If our house is on fire, we lit the match ourselves.
Heather Kaufman, DPM, Anchorage, AK
07/16/2025
RESPONSES/COMMENTS (PM ARTICLES)
From: Lawrence Rubin, DPM
A few weeks ago, I read a convincing article in Podiatry Management Magazine that portends podiatry's potential demise if there is continued low matriculation of students in our colleges. Then, a few days ago, I saw a LinkedIn post from APMA in which podiatrists attending a major convention were celebrating the fact that podiatry has never been more viable and successful than now and can look forward to a marvelous future.
While I have deep feelings wanting APMA and these podiatrists to be right, something tells me that we should not ignore our failure to attract students and the possible adverse consequences of this occurring.
Lawrence Rubin, DPM, Las Vegas, NV
07/04/2025
RESPONSES/COMMENTS (PM ARTICLES)
From: Joseph Borreggine, DPM
The recent article on the Stark Law is very important and informative for all medical providers to read and ultimately understand with respect to the day-to-day operations of running a medical practice, working cooperation as a medical referral source, as well as being an employee in a more than two person (group) medical practice. This law is meant to not only protect the Medicare system from fraud and abuse which can be deemed direct or indirect but also provide government regulation and guidelines preventing physicians from being paid inappropriately whether in a small group or larger corporate practice setting.
I commented on this subject a while ago in this publication and did not get one response; either because 1) every reader was either fully knowledgeable of what I was talking about or 2) was completely ignorant of my comments with respect to payment for “designated health services” (DHS) in a group...
Editor's note: Dr. Borreggine's extended-length letter can be read here.
07/03/2025
RESPONSES/COMMENTS (PM ARTICLES)
From: Paul Kesselman, DPM and Larry Kobak DPM, JD
In the June/July 2025 issue of Podiatry Management, the Legal Corner provides an excellent synopsis of Stark Law and how it can find its way into everyday podiatric practice. There is one point (Number 5), however, which requires clarification. Regarding DME, it states, "If you own a durable medical equipment company and refer a patient to that company," this could potentially be a Stark violation.
Providing DME to your own patients in your podiatry practice is an allowed exclusion under Stark, just as taking x-rays of your own patients is an exception under Stark. Further clarifying is that you and the doctor must perform the service. You cannot have someone in your office dispensing the DME, in particular if the DME is a designated health service, as AFOs, for example, are. Furthermore, if your employees are assisting in providing any designated health service (DHS), they must be performing this under your direct supervision, while you, the doctor, actually are in the office. There are certain DME (e.g. surgical dressings) which are not DHS, and all the Stark rules may or may not apply.
Furthermore, if you do own a legally identifiable DME company with a separate tax ID from your practice and you refer your patients there, that may be problematic. Under these circumstances, it is highly suggested that you consult with a healthcare attorney to ensure you are in compliance with all Federal Stark and Anti-kickback regulations. There are also other regulations, including state licensing requirements, facility accreditation, and surety bonding that likely will apply here, which again like Stark, DO NOT APPLY to physicians providing DME to their own patients as part of a treatment plan and within their scope of practice.
Paul Kesselman, DPM, Oceanside NY, Larry Kobak, DPM, JD, NY, NY
06/30/2025
RESPONSES/COMMENTS (PM ARTICLES)
From: Rod Tomczak, DPM, MD, EdD
If you read the recent article titled, “Our House is on Fire” in Podiatry Management, it’s probably because you have some interest in podiatric education. You still have a large loan for your education, you are looking to hire a new associate/partner, thinking about selling your practice to a future graduate, teach at one of the podiatry schools, are a podiatric residency director, or are a current podiatry student. That pretty much takes care of the whole profession and, I might sum it all up by stating, “You have a skin in this game.”
Dr. DeHeer reminded me that it’s easy to be a Monday morning quarterback when tragedy arises. Almost as easy as it is to scream, “Monday morning quarterback.” By now we expect more. Let me remind Dr. DeHeer that, as President of the APMA, he has moved through all the chairs and probably has some thoughts about podiatric education. I guess everyone missed the proverbial light at the end of the tunnel not being daylight but...
Editor's note: Dr. Tomczak's extended-length letter can be read here.
03/21/2025
RESPONSES/COMMENTS (PM ARTICLES)
From: Steven Finer, DPM
Yesterday, I received the March 2025 issue of Podiatry Management. A most important statistic in PM's Annual Survey Report showed the 1997 gross income as $268,000. Fast forward... it was the same for 2023. Adjustments for inflation should make it $453,000 dollars. A new car then was $19,000, a house $143,000. What do you pay for office rent in 2025, supplies, and salaries? In 1997, my office rent was $800. My secretary was paid $10 an hour. If you make $100 a week and bread is 25 cents, then all is well.
Steven Finer, DPM, Philadelphia, PA
03/18/2025
RESPONSES/COMMENTS (PM ARTICLES)
From: Steven Kravitz, DPM
Congratulations to my friend Paul Kesselman. Paul is a quiet, non-assuming professional who doesn't brag about his accomplishments. He simply continues his passion of informing podiatrists of the many different aspects and the changing environment that constantly occurs with billing - coding and related aspects.
As pointed out nicely in the post by Bruce Kaczander, DPM, Dr. Kesselman has undoubtedly helped countless numbers of podiatrists across the country for many years in this important aspect of medical practice. He has, in my opinion, been under-recognized for his contribution to our field. The readers of PM magazine got it right in giving him this award for the Hall of Fame. Well deserved. Expect to see more to come. With gratitude and a strong congratulations.
Steven Kravitz, DPM Winston-Salem NC area
03/17/2025
RESPONSES/COMMENTS (PM ARTICLES)
From: Bruce Kaczander, DPM
Congrats to my fellow ICPM ‘81 classmate, Paul Kesselman, on a well-earned and deserved honor. Hopefully, Paul, you realize that you have directly or indirectly helped every colleague throughout the country. How many other Hall of Famers can make that claim! Your Motown friend is proud of you.
Bruce Kaczander, DPM (retired)
11/19/2024
RESPONSES/COMMENTS (PM ARTICLES)
From: Keith L. Gurnick, DPM
Keith L. Gurnick, DPM, Los Angeles, CA
11/14/2024
RESPONSES/COMMENTS (PM ARTICLES)
From: Jeffrey Trantalis, DPM
I find a meeting on biomechanics is critical in the importance of caring for people, not only for the lower extremities. but even the lower back. The commercialization of store-bought orthotics is doing a disservice to the American public. Not only are the American people ignorant of the benefits of biomechanics, so is the medical community in general. After all, surgery is the main impetus for many of the surgical professions, not conservative care that might help many of these people.
Years ago, I had the opportunity to work for a back surgeon. What I learned in this short time was that people with hip or back pain were born with a limb-length difference (with or without a pelvic rotation), or it was acquired as we got older. I did not have the opportunity to perform studies showing these benefits. Nobody in academia was interested. Besides, surgeons are trained to perform surgery and their livelihood would be affected. We as podiatrists are trained in surgery as well as providing non-surgical treatments. I saw the benefits of our training while working at the University of Washington Sports Medicine Clinic and practicing in Florida among the elderly.
Jeffrey Trantalis, DPM, Retired, Delray Beach, FL
11/13/2024
RESPONSES/COMMENTS (PM ARTICLES)
From: Keith l. Gurnick, DPM
An accurate definition of the word "custom" (as an adjective) is something made to unique specifications, especially something one of a kind. Its synonym is "custom-made". A definition of "custom-made" is something made for a specific or a particular person or individual. A definition of a "specific or particular person" is of or relating to a single or specific person, rather than to others or all. There are numerous definitions of the word "orthotic".
Here are examples of some of them: An orthotic is an orthopedic appliance designed to straighten or support a body part. Another is a device or brace to control, correct, or compensate for a bone deformity. Still another I found is a shoe insert designed to improve posture, improve function, and prevent injury. I am certain our readers can find...
Editor's note: Dr. Gurnick's extended-length letter can be read here.
10/05/2024
RESPONSES/COMMENTS (PM ARTICLES)
From: Jon Purdy, DPM
This is yet another joke by Medicare on the unsuspecting. I believe it was 2021 when they changed the rules on the L1951 and probably some others. I’ve been burned by RAC for having dispensed these on patients such as those with CMT drop foot. I did my peer-to-peer to find out this new “rule” had been added buried deep in the layers of determinations and edits.
Pre-fabricated is just that, and by definition should not need “customization.” Yet a brace that fits perfectly as is, is no longer adequate if it is not “adjusted” in some fashion. It’s just getting ridiculous out here. But that’s the game. Change it up even if it makes no sense, they’ll miss it, and we can get them until they figure it out. Doctors and patients suffer because of it.
Jon Purdy, DPM, New Iberia, LA
10/03/2024
RESPONSES/COMMENTS (PM ARTICLES)
From: Paul Kesselman, DPM
There are several additional points one should understand when it comes to RAC and TPE. You are not being targeted; it is the code which is being audited and you have been the "lucky" one selected from a batch of several thousand claims.
Second and most important: A colleague from another healthcare profession and I recently commiserated on our experiences with unjustifiable denials as a result of RAC audits. We have both concluded that these judgments are stacked against the provider because the financial health of the RAC agency is wholly dependent on...
Editor's note: Dr. Kesselman's extended-length letter can be read here.
09/14/2024
RESPONSES/COMMENTS (PM ARTICLES)
From: Lawrence Kosova, DPM
Dr. Davis, there is a saying in AI, "AI won't replace doctors but doctors that don't use AI will be replaced." Being one of the podiatrists interviewed for the article, I wanted to comment. AI is really being used for most of us for increased efficiency and improvement, not replacement. If anyone will be replaced, the radiologists might be lessened in numbers.
The technology for breast cancer diagnosis and other cancers is really something, and using AI as an assistant for improved diagnosis is key. I am having an upcoming colonoscopy and the doctor is one of the leading specialist in this field is using AI as an adjunct. With AI, she has an increased finding of adenoma rate of 25% that might of been missed before this technology. Now all residents/fellows are being trained with...
Editor's note: Dr. Kosova's extended-length letter can be read here.
09/11/2024
RESPONSES/COMMENTS (PM ARTICLES)
From: Elliot Udell, DPM, Bruce Pinker, DPM
Dr, Davis may be concerned that computer technology may phase out some aspects of medicine. It is doubtful that it will affect podiatry. Until they invent a computer with two sets of four fingers and two thumbs, we will always be needed.
Elliot Udell, DPM, Hicksville, NY
Earlier this year, I completed a course for Artificial Intelligence in Healthcare through the Massachusetts Institute of Technology (MIT). Artificial Intelligence (AI) has several benefits, as well as drawbacks. Overall, it can facilitate processes, and these systems will likely improve in the future.
Currently, some operating rooms utilize AI systems to assist with scheduling to improve efficiency, and there is a report that ChatGPT helped to diagnose a neurological patient who had seen several doctors and finally received the proper treatment thanks to the assistance of AI. Also, there are AI systems that can help improve patient compliance in following a doctor’s orders in terms of taking medications properly, as prescribed. However, AI cannot function on its own - AI results must be reviewed and monitored to ensure accuracy.
Bruce Pinker, DPM, White Plains, NY
09/10/2024
RESPONSES/COMMENTS (PM ARTICLES) - PART 1B
From: Paul Kesselman, DPM
The article cited in a recent PM News edition requires some updating. Since it was written and published, CMS has made a change with respect to the process of prior authorization of bone stimulators. Due to some technical issues with various generations of this technology, CMS last week announced that they were halting the prior authorization process on bone stimulators. When enforcement of this process takes place, CMS promises to make another announcement.
Paul Kesselman, DPM, Oceanside, NY
09/10/2024
RESPONSES/COMMENTS (PM ARTICLES) - PART 1
From: Ali Davis, DPM
I just wanted to make a comment about the AI article recently written. I have explored AI in my practice but a big concern is the reason this is free or cheap to us is because they are planning to phase us out- we are feeding the computers the data and knowledge to phase us out- it is allowing computers to collect data and eventually a company will use this to charge patients money to diagnose and treat themselves- not good for our profession. I personally do not plan to use this technology as it is helping to phase out physicians. It is not good for our profession.
Ali Davis, DPM, Overland Park, KS
12/14/2023
RESPONSES/COMMENTS (PM ARTICLES) -PART 1
From: James Koon, DPM
I closed my practice 8 years ago to join a multi-specialty clinic. I got one records request in the 7 years I had to keep the records. One. I called the requestor and was released from it as my contribution was nominal. I simply kept my server. My vendor, MacPractice, assured me that IF I ever needed a chart, they would be able to pull it off my server no matter how many software updates transpired. For a fee. I never needed it.
We did have some residual paper charts that I rented a storage space for and pared them yearly. I paid to have them shredded. I also sold my x-rays for the silver recovery. Both were an expensive and laborious endeavor. In retrospect, I should’ve just had a big bonfire and partied with friends.
Closing a practice takes longer than you think and costs more than you think. Bills come out of thin air for months. Banking costs, vendor contract terminations, x-ray equipment decommissioning costs, files, legal notifications, etc. I don’t envy anyone doing it. I love being an employed physician.
James Koon, DPM, Winter Haven, FL
|
| |

|
|
|







