09/10/2013
RESPONSES / COMMENTS - (CLINICAL) - PART 1B
RE: Gangrene S/P Cast Complication
From: Wm. Barry Turner, BSN, DPM
It may already be too late, but I would try to instigate the use of oral and topical vasodilators. Using HBOT is a great idea, but keep in mind that O2 is a vasoconstrictor. The blood fluid will be richer in oxygen. If you couple the oxygen therapy with a vasodilator, you will see a much quicker and maximized response. I do not like the response quoted from the ortho doctor. I hope his licensing organization is aware of his callous concern for this patient. Topically, I would rub in 1/2 inch of nitroglycerin pasted to the affected foot's arch, tid. Hold for SBP under 100mm. Discuss with the patient's PMD about using oral medication, like Procardia.
My question to the patient's parent, "how did the child tolerate the significant pain that would accompany this travesty?"
Wm. Barry Turner, BSN, DPM, Royston, GA, claret32853@ymail.com
06/14/2013
RESPONSES / COMMENTS - (CLINICAL) - PART 1B
RE: Recurrent Ganglion Cysts
From: Steven J. Kaniadakis, DPM
Typically, I inject Depomedrol just proximal to the post-surgical wound. According to O.A. Mercado's videos, and other various reference textbooks, a "few drops of Decadron" intra-operatively is another technique. The post related to using "non-absorbable suture and to heavily cauterize it." I suspect that this might be causing further perpetuating aggravating factors such as the irritation of the surrounding structures, and causing the cycle to repeat from repetitive irritation of remnant sutures, perhaps overzealous necrotic cauterized tissue.
I would have selected an absorbable type suture to help nature maintain a smooth natural gliding action. If it's emerging from a (synovial) joint, then there may be iatragenic causes that are inducing tendon sheath ganglionic cyst(s). Finally, a firm compression post-op dressing helps with a mixture of long and short-acting corticosteroids.
Steven J. Kaniadakis, DPM, St. Petersburg, FL, stevenkdpm@yahoo.com
06/11/2013
RESPONSES / COMMENTS - (CLINICAL) - PART 1B
RE: Recurring Skin Lesions
From: Dennis Shavelson, DPM
This is a case of biomechanical surgical iatrogeny. These are not recurrent lesions as Name Withheld has labeled them; they are transfer lesions. The surgeon has stripped the distal segment of the 3rd digits in question from being functional in closed chain. The patient has morphed mechanically to a compensatory equilibrium via Wolf’s and Davis’ laws. That is giving a new location of the digits weight-bearing purpose which they are not biologically capable of assuming, resulting in this pathological dermatological reaction.
Perform a biomechanical evaluation of the digits, beginning with functional foot typing, and take a biopsy of the lesion. Send the specimen to a pathology lab (such as Bako) that can give you a biomechanical microscopic reading of the slide. Utilizing that data, develop a non-operative and/or operative plan of care to resolve this painful and disabling problem.
Disclosure: I am a consultant to Bako Labs.
Dennis Shavelson, DPM, NY, NY, drsha@foothelpers.com
06/10/2013
RESPONSES / COMMENTS - (CLINICAL) - PART 1B
RE: Recurring Skin Lesions
From: John Scheffel, DPM
It's hard to tell without x-rays, but I wonder if the initial surgeon performed a flexor tendon transfer instead of just a tenotomy? I had a similar case in which the proximal phalanx was causing a similar problem. The patient had the procedure done years earlier, and all that was left of the proximal phalanx was its base, which was sitting distal-plantar to the met head.
Excision of the base of the proximal phalanx with syndactylization to the adjacent digit addressed her pain.
John Scheffel, DPM, Worcester, MA, jscheffel@townisp.com
05/18/2013
RESPONSES / COMMENTS - (CLINICAL) - PART 1B
RE: Painful Bunion in a 12 Year Old
From: Name Withheld
Thank you to those who gave me your input. I did not provide an extensive biomechanical exam with my first presentation. This patient has at least 10 degrees of ankle dorsiflexion with her knee extended or flexed. Her hamstrings are not tight. She has symmetrical hip motion, more with no internal position. There is no internal tibial torsion. She does not have ligamentous laxity. Her first ray is stable on exam. She is only moderately pronated in stance and gait. Her lateral x-ray does not have an anterior break in the cyma line. There is no Kirby's sign. There is no elevation of 1st ray (Seeberg's index).
She has noticed the bunions for several years, and has had moderate aching in the joint for...
Editor's note: This extended-length letter can be read here
05/16/2013
RESPONSES / COMMENTS - (CLINICAL) - PART 1B
RE: Painful Bunion in a 12 Year Old
From: Gary W Docks, DPM
The metatarsus adductus and positive metatarsal protrusion factor highly when considering the bunion correction. One thing you did not mention is whether she had a significant equinus, which definitely is causal when you're looking at a juvenile bunion deformity. That being said, you must also be aggressive in choosing your procedure versus being conservative, which likely will result in a recurrence. Remember, the met adductus deformity will increase the IM angle. I therefore recommend the following procedures:
1. Endoscopic gastroc recession 2. Scarf or Austin Bunionectomy with screw fixation. There are still remnants of the growth plate at the base of the lst metatarsal. You could perform a Juvara, but you would have to be careful to avoid the growth plate. Remember to be aggressive and reduce the IM angle or 10 years from now, you'll be looking at a re-do.
Gary W Docks, DPM, Beverly Hills, MI, gwdocks@aol.com
05/11/2013
RESPONSES / COMMENTS - (CLINICAL) - PART 1B
RE: Overlapping 2nd Digit Status Post Bunionectomy
From: Don Peacock, DPM)
I wanted to show a nice correction I got on a bunion deformity with the patient on whom I felt uncomfortable with doing a 1st metatarsal osteotomy. In your case, you would have to remove the fixation in the first metatarsal. This can complicate the redo procedure for the patient. On the elderly patient, I’m going to show I performed a minimally invasive bunionectomy and Akin through and through.
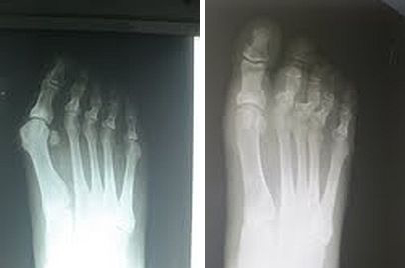 |
Pre- and Post-op X-Rays, Akin Performed Minimally Invasive |
I used the same incision percutaneously to perform the bunionectomy and the Akin. The interesting result with her x-rays is that...
Editor's note: Dr. Peacock's extended-length letter can be read here.
05/08/2013
RESPONSES / COMMENTS - (CLINICAL) - PART 1B
RE: Chronic First MPJ Pain (Don Peacock, DPM)
From: Sloan Gordon, DPM
Dr. Peacock, your x-rays are most impressive. You plantarflexed the first ray below the dorsal cortex, which will off-load the first ray, and you removed the 1st MTPJ exostosis just perfectly. I am not sure how you did this through a 1.5 cm incision, unless this was MIS. I guess we Texans like things big, including our incisions!
If this was MIS, I would be concerned about a non-fixated metatarsal osteotomy along with the gastoc lengthening. It seems like taking a risk for displacement of the osteotomy. But, the pre- and post-operative films are impressive. If this was MIS, why not drive a percutaneous 0.062" Kirschner wire through the osteotomy? I am certainly not faulting your technique!
Sloan Gordon, DPM, Houston, TX, sgordondoc@sbcglobal.net
05/04/2013
RESPONSES / COMMENTS - (CLINICAL) - PART 1B
RE: Post-Keller Complication (Gregory Caringi, DPM)
From: Don Peacock, DPM
Unfortunately, this case is a result of an inappropriate procedure performed on a 54 year-old patient. Keller procedures should be used with caution and have a significant history of complications. In Keller’s original paper, he discussed that he also performed an extensor hallucis longus lengthening. This is overlooked by some surgeons. Kellers are intended for use in the elderly.
Two of the most significant deformities resulting from Keller procedures are...
Editor's note: Dr. Peacock's extended-length letter can be read here.
04/25/2013
RESPONSES / COMMENTS - (CLINICAL) - PART 1B
RE: Post-Op Hallux Varus (Kel Sherkin, DPM)
From: Robert Bijak, DPM, Jeffrey Kass, DPM
Simply correct the PASA with a Reverdin.
Robert Bijak, DPM, Clarence Center, NY, rbijak@aol.com
If there is no pain, then of course one doesn't have to repair it. The patient does have a complaint and if you to chose to address it, you may want to consider the Arthrex mini tight rope. I would like to add, a podiatrist could have had the same outcome.
Jeffrey Kass, DPM, Forest Hills, NY jeffckass@aol.com
04/24/2013
RESPONSES / COMMENTS - (CLINICAL) - PART 1B
RE: Post-Op Hallux Varus (Kel Sherkin, DPM)
From: Ira Weiner, DPM
Based upon the x-ray findings and history, I feel a closing Aiken osteotomy is in order. Since she states that the MPJ has a pain-free ROM, I would not address that. It appears she does not have the classic "staked" metatarsal. If a fusion procedure is warranted in the future, there is plenty of good bone left to support that procedure using any fixation method of choice.
As a side note, the question of cosmesis only is brought up. I feel if she has difficulty finding the shoes she wants, it becomes her call as to whether or not she wants this corrected. I don't feel there is a single surgeon among us who does not strive for good cosmesis in an elective procedure. Salvage procedures are a little different. If the patient is unhappy with the way the procedure looks, then we have a duty to correct the problem if it's something we are able to do.
Ira Weiner, DPM, Las Vegas, NV, vegasfootdoc2005@yahoo.com
04/20/2013
RESPONSES / COMMENTS - (CLINICAL) - PART 1B
RE: Bacterial Infection of Nail (Jay Kerner, DPM)
From: Martin V. Sloan, DPM
I had similar reported findings after I submitted a nail specimen to a major pathology lab to rule out onychomycosis. The report said "bacterial overgrowth with no fungal elements seen," and identified this same staph organism, Staph hemolyticus. The patient acquired her condition at a nail spa and wanted it resolved. So I put her on an appropriate anti-staph antibiotic (not Cipro) for a time, and the condition resolved. I don't know whether it was a colonization or an infection, but that debate could be extended to the dreaded fungal toenail as well.
Martin V. Sloan, DPM, Rowlett, TX, martinsloan@me.com
04/19/2013
RESPONSES / COMMENTS - (CLINICAL) - PART 1B
RE: Wart Covered Foot (David Kahan, DPM)
From: Philbert Kuo, DPM, Brian Kiel, DPM
This looks like a good case for the Panacos procedure. David Secord, DPM has discussed this procedure and Peter Bregman, DPM has written about it.
Philbert Kuo, DPM, Chesapeake, VA, philbertkuo@gmail.com
With patients like this I have successfully treated the condition with once daily applications of 10% formalin solution (formerly Lazerformalyde) which can be made by your local pharmacy and 1200 mg of cimetidine (Tagamet) given in a single or divided dose. I see them after 3 weeks for debridement and then every 6 weeks. I have seen this be successful in a matter of weeks, but usually it takes 4-8 months.
Brian Kiel, DPM, Memphis, TN, Footdok4@gmail.com
04/17/2013
RESPONSES / COMMENTS - (CLINICAL) - PART 1B
RE: Unresponsive Vesicular Dermatitis (Mark Aldrich, DPM)
From: Sloan Gordon, DPM
I suggest avoiding the potent topical steroids as their mechanism of action is vasoconstriction. I have had success with Pimecrolimus cream (a steroid-free medication applied to the skin). Also, there is a causal relationship with eczema and low levels of Omega 3s, so I would try some OTC or Rx Omega 3.
Sloan Gordon, DPM, Houston, TX, sgordondoc@sbcglobal.net
04/08/2013
RESPONSES / COMMENTS - (CLINICAL) - PART 1B
RE: Recalcitrant Heel Pain (Loren J Miller, DPM)
From: Jeff Root
One other possible etiology that hasn’t been mentioned for Dr. Miller’s patient with recalcitrant plantar heel pain is atrophy of the plantar fat pad. When Dr. Miller said that his patient’s pain is directly beneath the heel tubercle, are we to assume he was referring to the medial tubercle? There are a number of biomechanical factors to consider. Individuals with a cavus foot can function excessively supinated or pronated, which can cause compression and atrophy of the medial (excessively pronated foot) or lateral (excessively supinated foot) plantar fat pad. A gait analysis can reveal if...
Editor's Note: Mr. Root's extended-length letter can be read here.
04/05/2013
RESPONSES / COMMENTS - (CLINICAL) - PART 1B
RE: Recalcitrant Heel Pain (Loren J Miller, DPM)
From: Gino Scartozzi, DPM
The patient appears to have recalcitrant heel pain despite the numerous conservative and surgical treatments employed. In light of the posting of treatments thus far offered, I suggest two follow up approaches in conjunction with post-operative orthotic therapy which I assume is continuing.
First, a full arthritic profile should be performed to see if there is a systemic arthritic condition that is contributory to his heel pain. The profile should consist of a sedimentation rate, HLA-B27, uric acid, rheumatoid factor and ANA. If these factors test positive, appropriate referral to a rheumatologist may be required.
Second, does the patient exhibit lower back symptomatology. Lower spinal segment impingements can also contribute to recalcitrant heel pain. Physical therapy and/or chiropractic care is essential after MRI assessment of such pathology.
Gino Scartozzi, DPM, New Hyde Park, NY, Gsdpm@aol.com
04/03/2013
RESPONSES / COMMENTS - (CLINICAL) - PART 1B
RE: Post-op Varus (Joshua Kaye, DPM)
From: Don Peacock, DPM
This is a perfect case that could easily be handled with minimally invasive surgery. The correction of hallux varus by implant can be doomed to failure in many cases because underlying biomechanical issues causing the deformity will not be addressed. I have tried to correct hallux varus with implant surgery and have also had less than favorable results. I have abandoned the use of implants to correct hallux varus.
The patient that you present would be a good candidate for a reverse minimally invasive Akin osteotomy. This osteotomy could be performed even now despite the fact that an implant is in place. The placement could be made just distal to your current implant. Also, the second and third toes could be corrected utilizing a wedge osteotomy of the proximal phalanx directing the toes more laterally. This could be achieved utilizing a minimally invasive surgery known as the Isham hammertoe correction.
I was trained traditionally and would have approached this deformity much in the way you have until more recent years in which I have utilized minimally invasive surgical techniques. These techniques are especially good for use in the elderly and for performing re-do surgery. I am a board-certified foot surgeon by ABPS, but have gone against the grain and incorporated minimally invasive surgery into my practice with absolutely stunning results.
Don Peacock, DPM, Whiteville, NC, peacockdpm@gmail.com
03/12/2013
RESPONSES / COMMENTS - (CLINICAL) - PART 1B
RE: Efficacy of Laser for Onychomycosis (Tip Sullivan, DPM)
From: Keith D. Sklar, DPM
I’d like to share my experience on the use of lasers with nail fungus. I use my laser as one segment of my treatment protocol to clear and maintain a healthier nail plate. I also address the surrounding skin. I have found that to take a dystrophic nail plate and convert it to a healthy nail plate is a long-term process. I inform all my patients that they must be very patient and compliant. We discuss a custom pathway and treatment plan that will address their condition, providing the patient with the most optimal results available.
In moderate to severe cases, my treatment consists of the use of the laser and topical medications. We do employ an oral medication. Once the treatment plan has been made, the process of...
Editor's note: Dr. Sklar's extended-length note can be read here.
03/11/2013
RESPONSES / COMMENTS - (CLINICAL) - PART 1B
RE: Efficacy of Lasers for Onychomycosis (Adam Landsman, DPM)
From: Paul J. Maglione, DPM, David Zuckerman, DPM
Having had a laser for a year and a half, I have kept my own statistics: 1) For long-standing mycotic toenails (onychauxic type), the nails will thin out. However, they will not become the "thin, pink type." The result will please patients. 2) For recent infections, the results are gratifying to both the patient and myself. 3) Nails must have a positive fungus culture; the laser will do nothing for psoriatic nails. 4) Technique is very important. Any missed portions of nail will affect the result. 5) I do not use a topical concurrently. Based on laser physics, this may or may not affect the action of the laser. Dr. Zuckerman can weigh in on this.
Paul J. Maglione, DPM, Ossining, NY, drmaglione@aol.com
It’s important to first acknowledge that any type of laser treatment for fungus toenails is not a miracle cure. We need to continue to develop the research investigating laser treatments in order to determine the exact mechanisms of action, how we can improve outcomes, what the biomechanical and structural role of the foot is, and how it affects outcomes, as well as to examine the systemic implications of laser treatments, i.e., auto-immune disease, diabetes, etc.
I was surprised that Dr. Landsman believes that heat plays the primary role in destroying fungus, especially given his research with the laser company Normir in photo-inactivation along with...
Editor's note: Dr. Zuckerman's extended-length letter can be read here.
03/08/2013
RESPONSES / COMMENTS - (CLINICAL) - PART 1B
RE: Numbness in Foot When Driving (Olga Luepschen, DPM)
From: Richard A. Simmons, DPM, Paul Busman, DPM, RN
Many men carry a wallet in one of their back pockets. If this is the case, have him remove the wallet when driving and/or sitting.
Richard A. Simmons, DPM, Rockledge, FL RASDPM3955@gmail.com
Is this on the side of the pocket where he carries his wallet? We all have so many credit cards, etc. that a man's wallet can approach 2" in thickness, putting a lot of pressure on the sciatic nerve roots. I had a very similar problem myself, until my chiropractor suggested removing my wallet from my pocket when I drive. I'm not sure how taking his foot off the pedal and moving it helps, unless he's also unloading the wallet area. Now, I carry an innovative wallet called the All-ett (for which I have no financial interest). It redistributes credit cards, license, store premium cards, etc. into a much thinner profile.
Paul Busman, DPM, RN, Clifton Park, NY, paul@busmanwhistles.com
03/02/2013
RESPONSES / COMMENTS - (CLINICAL) - PART 1B (CLOSED)
RE: Fixation Vs. Non-Fixation of Osteotomies (Gino Scartozzi, DPM)
From: Lawrence Kobak, DPM, JD
I thought it was very interesting that one podiatrist cited Dr. Mercado as an excellent surgeon and example. Dr. Mercado has lectured for the Academy of Ambulatory Foot Surgery and in his excellent books, he has described several minimal incision techniques that he himself used! In the other letter published, somehow I am taken to task about local vs. national standards. I simply never wrote that. However, as a healthcare attorney, I enjoyed the lecture by someone with no legal training. The letters are filled with conclusory "observations" and war stories. Practices "market" themselves that utilize all types of incisions and surgical techniques.
Additionally, there happens to be a breadth of literature on non-fixated osteotomies, if the...
Editor's note: Dr. Kobak's extended-length letter can be read here. This topic is now closed and no further letter will be accepted or published.
02/23/2013
RESPONSES / COMMENTS - (CLINICAL) - PART 1B
RE: Fixation Vs. Non-Fixation of Osteotomies (Ed Cohen, DPM)
From: Don Peacock, DPM
I agree with Dr. Cohen's position on non-fixated osteotomies of digits and lesser metatarsals. I am ABPS board certified and was trained in conventional surgery. In recent years, I have incorporated MIS techniques into my surgical arsenal. In my opinion, one of the reasons for complications following lesser metatarsal osteotomies is not that we perform too many of these procedures, but that we only partly correct metarsalgia with metatarsal osteotomies.
I routinely perform lesser metatarsal osteotomies on mets 2-4 at the same time via MIS techniques and allow the mets to seek their own level without fixation. So far, I have not had AVN or non-union as a complication. Transfer lesions have also been eliminated as a complication. In the last several years, I have corrected all Tailor's bunions via MIS osteotomy without fixation and have had no incidence of non-union. In fact, the only case I have ever had AVN was in an Austin procedure in which I used screw fixation. The 1st rays I have non-fixated have all healed so far.
Don Peacock, DPM, Whiteville, NC, peacockdpm@gmail.com
02/21/2013
RESPONSES / COMMENTS - (CLINICAL) - PART 1B (CLOSED)
RE: Etiology of Hallux Varus (Dennis Shavelson, DPM)
From: Robert Bijak, DPM
If we accept Dr. Shavelson's theories, then nearly all podiatrists and podiatry school biomechanics are wrong, and we have been treating patients unsuccessfully for a generation. Where are the biomechanic experts from our hallowed institutions to tell us who's right? Or, do they also believe orthotic biomechanics is so much alchemy?
Robert Bijak, DPM, Clarence Center, NY, rbijak@aol.com
Initially, this discussion started with what appeared to be a case of idiopathic hallux varus. Now, it has progressed or digressed into a discussion on the basics of what I like to call BIOMAGIC. Root vs. Shavelson (FLEB). I do not claim to be a biomechanics expert or an innovative thinker. I do claim to have years of experience in surgery which requires a sound understanding of the way the foot works. What is successful in some does not work in others.
Biomechanics principles should be used as a teaching tool for...
Editor's note: Dr. Sullivan's extended-length letter can be read here.
02/16/2013
RESPONSES / COMMENTS - (CLINICAL) - PART 1B
RE: Etiology of Hallux Varus (Dennis Shavelson, DPM)
From: Eric Fuller, DPM
Dennis Shavelson, DPM wrote: "Hallux valgus occurs in the flexible forefoot functional foot types, with few exceptions. As Dr. Fuller mentions, this foot type characteristically is attached to an inhibited (exhausted), poorly leveraged, poorly trained peroneus longus muscle engine that cannot oppose the increased dorsiflectory stiffness of the first ray that exists in this foot type."
Dr. Shavelson, I never said anything like that. I've examined your foot typing system and would not use it to characterize this situation. Also, the rest of your statement doesn't make any sense. Please quote me correctly.
Eric Fuller, DPM, Berkeley CA, fullerpod@gmail.com
02/15/2013
RESPONSES / COMMENTS - (CLINICAL) - PART 1B
RE: Etiology of Hallux Varus (Jordan Sheff, DPM)
From: Ed Cohen, DPM
When I wrote about doing a reverse Reverdin-Isham procedure with lateral 1st metatarsal head and hallux osteotomies as well as straightening toes 2-4 with lateral proximal base phalangeal osteotomies, I should have said the patient will probably need to be followed up with a pair of orthoses.
I feel it is important to do the surgery because the orthotic control is not enough to solve the shoe problem of the crooked toes, just as an orthosis will not correct an HAV deformity, but can be very helpful after surgery by controlling some of the abnormal factors contributing to the deformity.
Ed Cohen, DPM, Gulfport, MS, ecohen1344@aol.com







