





|

|
|
|

|
Search
12/28/2016
RESPONSES/COMMENTS (CLINICAL) - PART 2A
From: Dennis Shavelson, DPM
When performing bunion surgery, there are two important caveats: Caveat #1. The sesamoid apparatus must be positioned in the correct anatomical alignment in relation to the first metatarsal head. There is very little tolerance to this rule. Caveat #1 is folkloric at best. I have a desire to hold Dr. Fellner to the same standards that you are asking Dr. Peacock to uphold. Is there any evidence or peer-reviewed literature proving that poor sesamoidal placement is of primary importance in selecting bunion procedures?
Caveat #2. the sagittal alignment of the first metatarsal must be balanced correctly with the lesser metatarsals. This requires of a surgeon a need to exercise due diligence intra-operatively to evaluate and adjust, as required. The sagittal plane alignment of the 1st metatarsal to the lesser mets is more than folkloric, but difficult to accomplish no matter what approach or procedure is selected to repair a bunion deformity. My questions here are: 1. Where does the evidence lead us in accomplishing this caveat? 2. is there evidence that we can balance the first metatarsal to the lesser metatarsals long-term?
Dennis Shavelson, DPM, NY, NY
Other messages in this thread:
03/13/2024
RESPONSES/COMMENTS (CLINICAL) - PART 2A
From: Jeff Root
Regarding the query about the treatment of recalcitrant "posterior tibial tendonitis", or what many would call posterior tibial tendon dysfunction (PTTD), I would like to share a few of my thoughts. The PM News subscriber stated that the patient wears "HOKA shoes and custom orthotics". The term "custom orthotics" simply implies that the devices were not prefabricated. In some cases, the lines between custom and prefabricated shoe inserts have been intentionally and unintentionally blurred. In addition, the term "custom orthotics" tells us little to nothing about the nature (i.e. design and properties) of the orthoses because there are hundreds if not thousands of types of custom orthotics and orthotic designs.
For example, what was the position of the joints of the foot, including the STJ, MTJ and 1st ray when the foot was casted or scanned? What were the specifications of the orthotic prescription? What lab techniques were used in creating...
Editor's note: Jeff Root's extended-length letter can be read here.
09/10/2020
RESPONSES/COMMENTS (CLINICAL) - PART 2A
From: Stephen Musser, DPM, Richard M. Maleski, DPM RPh
An additional x-ray view would be helpful. Addressing the contracture at the MTP is critical either with a Weil and/or soft tissue release. Equally important is the the use of a toe splint(s), Darko, used afterwards to keep the digits in a corrected alignment for the soft tissue to heal/scar down the toe in the desired position, with proper alignment until scar tissue and adhesions are formed.
Stephen Musser, DPM, Cleveland, OH
I agree that transverse plane deformity of the lesser digits is very hard to correct and have always tried to avoid surgery for these. In one case that was successful, in addition to PIPJ fusions of the 2nd and 3rd toes with pin fixation across the MTPJs, I performed capsulotomies and capsulorraphies of the MTPJs as well as base wedge osteotomies of the 2nd and 3rd metatarsals to correct for the small amount of met-adductus that was present. I also freed up the extensor tendons from the insertion to about the metatarsal neck area, and sutured the tendon sheath apparatus in a more medial alignment, to try to relieve the lateral pull of the tendon across the MTPJ.
I followed the patient, who was very active, for 4 years until I retired. At least until then, the correction held up very well and the patient was happy. I can only hope that the correction will continue to last. This is the only time I performed this combination of procedures and I think that the correction of the met-adductus, although seemingly minimal, was key.
Richard M. Maleski, DPM, RPh, Pittsburgh, PA
02/08/2019
RESPONSES/COMMENTS (CLINICAL) - PART 2A
From: Elliot Udell, DPM
Drs. Albritton and Jones show that there are multiple ways to skin a cat. In this case, the cat is the treatment of Raynaud's phenomenon. As Dr. Jones indicated, some people are hesitant to take an oral medication that is off-label for Raynaud's but FDA-approved for the management of hypertension. In our practice, we have done well with recommending disposable shoe warmers that are sold in sporting goods stores. Patients buy a box of them in December and it lasts until the spring. For others, we have successfully prescribed long-acting nifedipine. These patients take one pill a day starting in December and discontinue the drug when spring arrives. We check blood pressures on these patients before starting the drug to make sure they do not have hypotension and when they start, they are advised not to get up from a sitting position too quickly.
Two important points to consider are: 1) If the patient is taking other medications for hypertension, adding on nifedipine or the meds recommended by Dr. Albritton could cause an abnormal drop in the patient’s blood pressure. In those cases, it is wise to coordinate treatment with the patient's primary care physician. 2) Order an ANA on patients presenting with symptoms for the first time to rule out the possibility of scleroderma or lupus.
Elliot Udell, DPM, Hicksville, NY
10/31/2016
RESPONSES/COMMENTS (CLINICAL) - PART 2A
From: Dennis Shavelson DPM
I rarely disagree with Dr. Markinson, but his comments reflect the views and morays of “maximal” incision foot surgeons that need discussing. Dr. Peacock is an ABPS-certified surgeon who has become a “hybrid” surgeon by adding minimally invasive procedures to his toolbox. These procedures with rare exceptions, when well selected, take less time to perform (his point), allow ambulation earlier than traditionally recommended, heal faster, rehab functionally, and infect less often. In addition, the ability to control the post-op course biomechanically utilizing external biomechanical fixation apply Wolf’s and Davis’ Laws of adaptation better than rigidly fixated osteotomies and plated joints.
The worldwide acceptance on minimally invasive foot surgery because of reduced cost, shorter op time and the comparable results in many instances to procedures performed open are evident to those with an open mind to those moments when a new paradigm may actually be an advance to what “we have been fed for the last 35 years.” To quote Eric Hirzel, “The strength of one’s opinion should not exceed their knowledge on the matter.”
Dennis Shavelson DPM, NY, NY
08/31/2015
RESPONSES/COMMENTS (CLINICAL) - PART 2A
From: Elliot Udell, DPM
In the context of this academic discussion, none of us should diminish the honor and respect we all have for you and many of our other esteemed colleagues who keep biomechancics and foot orthotics on the front burner at our conventions. When I went to school at NYCPM, back in the 1970s, there were conflicting opinions between the late great Drs. Schuster and Dr. Root. Both men taught all over and had their myriads of followers as well as labs that produced their orthotics. These pioneers of biomechanics were respected more because of who they were rather than on well written academic papers published akin to what Wrobel and his team wrote.
As Dr. Kesselman points out, the opinions of podiatrists with high stature is not enough in this century to convince insurance companies to pay for orthotics. These people want to see current, well-written research papers. Unless we continue to invest in these studies, we cannot and should not expect anyone either in the insurance industry, orthopedics, or even well educated patients to believe that when we cast or scan patients in our offices for custom foot orthotics, we are not doing any more for them than what Dr. Scholls does when it has people stand on scanners at Walmart and take home pre-fabs.
Elliot Udell, DPM, Hicksville, NY
08/28/2015
RESPONSES/COMMENTS (CLINICAL) - PART 2A
From: Paul A. Galluzzo, DPM
I agree with Dr. Dockery and would like to thank him for his expertise on this subject. I have been using 4% alcohol injections for over 14 years and wish I would have started sooner. I mostly use them for neuromas and Baxter's nerve entrapment. I believe this treatment should be offered as another form of conservative treatment as most patients prefer to avoid surgery. I have heard patients tell me that they have gone to other podiatrists and were told that it doesn't work or that the podiatrist didn't believe in the treatment. I'm not sure how you can believe in something you don't utilize!
We are doing a disservice to our patients by not offering all forms of conservative treatments. I don't need studies to tell me this procedure works when I can see the results and I get referrals. If you don't use this treatment for whatever reason, send your patient to someone who does. I'd be more than happy to treat your patients. In the worst case scenario, it may not work (unlikely as it has an 80+ % success rate), and then surgery may be indicated.
Paul A. Galluzzo, DPM, Rockford, IL
03/27/2014
RESPONSES/COMMENTS (CLINICAL) - PART 2A
From: Adam Ullman
We have had many doctors indicate that they see a 15-20% increase in the efficacy of their laser treatments when their patients diligently use a SteriShoe sanitizer. When we have asked how they quantify this, it’s a bit of a guess. With that said, we know the fungus is in the shoes.
Novartis’s Lamisil study showed that the fungus is in the carpets and showers. While that may be true, we don’t spend 8-12 hours a day in one spot on our carpet or in our shower; however, we do spend 8-12 hours a day in our shoes. Every step compresses the sock, squeezing the fungus-laden sweat between the foot and the shoe.
It’s important that any protocol for onychomycosis not forget about the shoes. Socks end up in the washing machine, but shoes do not. The shoes need to be sanitized. Telling patients to throw out their shoes has one big problem – when will they contaminate their new shoes? Lysol and other chemicals, other than not being testing in shoes, pose health risks and contain warnings about use on clothing and contact with skin. A study with the SteriShoe sanitizer was published in JAPMA in the July/Aug 2012 issue. The article cites several other articles indicating that footwear is contaminated.
Disclosure: Shoe Care Innovations, Inc. is the manufacturer of the SteriShoe sanitizer.
03/26/2014
RESPONSES/COMMENTS (CLINICAL) - PART 2A
From: Keith Sklar, DPM
The question asked, “Has Laser Nail Fungus Removal Been Proven Effective?” I think this is a confusing question. The question should be, “Does the laser play an effective part in clearing dystrophic nails?” In my experience, the answer is a definitive YES. I have treated hundreds of patients with my laser and have achieved impressive results.
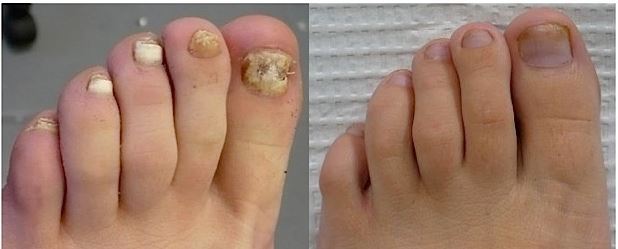 |
Before and After Photos Supplied by Dr. Keith Sklar |
In a previous post, I shared my experience on the treatment of dystrophic nails. The laser is only a part of my treatment plan to clear and maintain a healthier ...
Editor's note: Dr. Sklar's extended-length letter can be read here.
03/25/2014
RESPONSES/COMMENTS (CLINICAL) - PART 2A
RE: Has Laser Nail Fungus Removal Been Proven Effective? (Elliot Udell, DPM)
From: Ben Pearl, DPM
Dr. Udell raises a very legitimate concern. When the NY Times comes out with a position, people take notice. I am interested to hear if anyone has information on the specifics of the in-vivo results of the October 2013 article in the Journal of American Academy of Dermatology by Carney, et al. which was mentioned. Media information is all over the map. Not long ago, Consumer Reports put out a number of 90% effective treatment of laser on toenails with onychomycosis. The literature is also all over the map. Noguchi in 2013 reported a 27% decrease in turbidity, which was much less than many industry-backed studies. I look forward to having the profession continue to wade through this complicated data comparison to develop a reasonable consensus for how effective the laser is.
As just one small anecdotal data point, I have had lasers help my own nails, and some of my patients and I have had failures. I have come to my own conclusion that much of the success is driven by the physiology of the nail bed and immune status of the patient you are treating .
Ben Pearl, DPM, Arlington, VA, abenpearl@netscape.net
02/20/2014
RESPONSES/COMMENTS (CLINICAL) - PART 2A
RE: Non-Healing Wound S/P Neuroma Surgery
I performed a neuroma excision in November. I felt the resident did not evert the skin edges, but I let it go. The wound failed to close at eleven days. Local care was fruitless, so I revised the edges, antibiosed, and attempted a second primary closure.
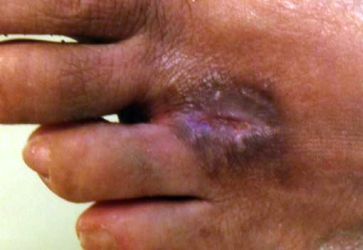 |
Post-Neuroma Dehiscence |
When the wound opened again, I began to shift blame to the patient's diabetes and smoking. In January, I performed an Integra procedure. Now, a month later, the wound is almost closed.
02/19/2014
RESPONSES/COMMENTS (CLINICAL) - PART 2A
From: Robert Bijak, DPM, Peter Bregamn, DPM
Assuming labs are normal (esp thyroid, glucose, C&S, plus additionally a vascular ck), re-cut out the margins and re-suture the fresh wound. Based on her weight, consider using a non- weight-bearing device .
Please make sure you take a proper culture, biopsy the tissue, and get an MRI. If the wound is clean, I recommend using multiple injections with amniotic fluid which will heal it in a couple of weeks if kept clean.
02/08/2014
RESPONSES/COMMENTS (CLINICAL) - PART 2A
From: Coyle DeMoss, DPM, Roody Samimi, DPM
I have seen many of these in the last 40 years of practice. It always did not seem to matter about the severity of the fracture or the plane of the break. Many treatment plans have been suggested, not the least of which is wiring the segments back. My experience has shown that the most effective and successful way is to meticulously excise the sesamoid, leaving all soft tissue as close to intact as possible. This solves the problem without fear of hallux deviation. A sharp 15 blade is the best solution to a chronic problem.
Put the patient in a BK cast for 3 to 4 weeks, then switch to a dancer's pad. If he is still symptomatic after three months, do a bone scan to check if there is delayed union. It won't hurt to try bone stimulation, but do this in a cast while the foot is immobilized. If still symptomatic, resection of the entire sesamoid from a plantar (vs. medial) approach may be more practical. I wouldn't worry about hallux deviation if you can stitch the capsule on that medial side, and get some scarring medially. But of course, make the patient aware that this could still happen.
02/07/2014
RESPONSES/COMMENTS (CLINICAL) - PART 2A
From: Evan Meltzer, DPM
Check out the following article: Zelen, CM, Poka, A, and Andrews, J. “Prospective, Randomized, Blinded, Comparative Study of Injectable Micronized Dehydrated Amniotic/Chorionic Membrane Allograft for Plantar Fasciitis- A Feasibility Study." Foot Ankle Int published online 14 August 2013.
12/10/2013
RESPONSES/COMMENTS (CLINICAL) - PART 2A
RE: First Ray Instability
From: Don Peacock, DPM
Judging from your patient's weight-bearing lateral x-ray, it does not appear that a hypermobile first ray is the issue. Her first metatarsal declination angle and talar tilt are relatively parallel on your weight-bearing lateral. Based on this x-ray, she appears to have a stable rear foot and a flexible forefoot. This type of case can be confusing because on the AP x-ray, she appears to have a long first ray. This could be that she, in fact, does have excessive dorsiflexor movement in the first ray which would appear as a long ray on an AP x-ray. However, it does appear that she is not overly flexible in the first ray based solely on the lateral x-ray.
A biomechanical exam will determine how flexible her forefoot is. She most likely has a rigid or stable rearfoot and flexible forefoot. If this is the case, then your surgical ideas would make perfect sense. A decompression osteotomy of the first ray along with orthotic use should suffice. Other options would be to perform a subtalar joint stabilization procedure if her forefoot is flexible. Both options would give advantage to the peroneal longus tendon, allowing for plantarflexion of the first ray. It is also important that you determine whether or not equinus is present.
Perform a distal metatarsal osteotomy in a decompression fashion and an osteotomy in a Bonney-Kessell style in the hallux. I would not address the mobility of the first ray unless there was true flexibility in the biomechanical exam or if she has gastroc equinus.
10/14/2013
RESPONSES/COMMENTS (CLINICAL) - PART 2A
From: Todd R Stewart, DPM
Having an implant fracture is not that rare an occurrence. We have all seen screws, plates, K-wires, and in this case, nitinol implants fracture. These can fracture for various reasons: defective implant, early unguarded weight-bearing, trauma, or surgeon error in inserting the implant.
In this case, both arms of the second toe implant and also a fractured arm of the third toe implant are noted. If there is mal-alignment or pain, the implants should be removed. The technique employed should be...
Editor's note: Dr. Stewart's extended-length letter can be read here.
10/12/2013
RESPONSES/COMMENTS (CLINICAL) - PART 2A
From: David Weiss, DPM, Joel Feder, DPM
I have put in hundreds of SmartToe implants, and typically have great success. However, sometimes they have fractured. I find it is imperative that a good bone-to-bone approximation is important to obtain good results. In addition, osteoporotic/osteopenic bone is not ideal for this fusion modality. It appears the problem here was a pseudarthrosis - fibrous union or possibly non-union. In order to repair this, I approach it typically as any other failed hammertoe fusion. Once the PIPJ is exposed, there would typically be significant fibrous material in the area. Pull the PIPJ apart, and grab the implants with hemostats. They should come out easily. Then revise the fusion site and use conventional pins. Sometimes I'll use cannulated screws form the distal phalanx to the proximal phalangeal base. If length is an issue, bone grafts could be used. Finally, a nice "compliancy" talk with the patient would be in order!
Unfortunately, we have encountered the fracturing of these implants several times in our personal and colleagues' cases, especially with dancers and runners. I don't think the SmartToe is perfected for use in active patients. Our solution has always required removal.
09/26/2013
RESPONSES/COMMENTS (CLINICAL) - PART 2A
RE: Unstable Scar
From: John F. Swaim, DPM
After ruling out osteo, vascular compromise, and skin cancer, place the patient in a TCC for 6-8 weeks, removing and debriding the area Q2 weeks. If he can revert this to intact skin, use a multi-density diabetic insole with additional layers of materials and a higher durometer outer shell to accommodate this larger patient as the usual thicknesses found in approved diabetic insoles would be meager and inadequate in this individual.
The Achilles lengthening likely aggravated the heel. Add onto the shoe or CROW-walker outsole an 3/8" heel lift and counter. Adjust the thicknesses by using a pressure plate to verify pressure reduction by at least 1/2 at the heel. Add mid arch PPT layers to augment, as needed.
A daily emollient will maintain the skin. If he has any fat pad left, I would try Tubi-grip, worn daily, or one of those new plantar fasciitis sleeves. The compression might be enough to limit the lateral excursion and tensile strain of the remaining fat pad and overlying skin, allowing for more cushioning of the area during ambulation. If the skin is unable to heal, I'd move to a round of debridement, then apply ACELL before taking this patient to surgery for a graft or flap.
03/20/2013
RESPONSES/COMMENTS (CLINICAL) - PART 2A
RE: Forefoot Surgery on an 84 Year Old (Joseph Borreggine, DPM)
From: Barry Mullen, DPM, Neil Levin, DPM
What you describe is more of a textbook repair for a young, active individual. Yes, we're all taught to treat physiologic rather than chronologic age...but, I'd still be concerned about compromised healing of multiple osteotomy sites. How active is this 84 year old? How severe are the symptoms? My gut thought is if surgery is necessary, a 1st MTP fusion and Clayton-Hoffman pan met head resection, with appropriate digital arthroplasty where necessary, would serve a patient of this age and that deformity well, with far reduced risk.
Barry Mullen, DPM, Hackettstown, NJ, yazy630@aol.com
Dr. Borreggine failed to provide any general medical history information that might play into the decision-making in an 84 year old patient. Let's look at the risk vs. reward ratio. If his chief complaint is the hammertoe, I would amputate the 2nd digit, leaving a small buttress of toe to prevent further medial migration of the lesser digits, and call it a day. If you sit down with the patient and truly discuss the possible morbidity of all that you are describing, I venture to say he would go for the amputation, and be back in a regular shoe in 2 -3 weeks.
Neil Levin, DPM, Sycamore, IL, DRFEET1@aol.com
|
| |

|
|
|







